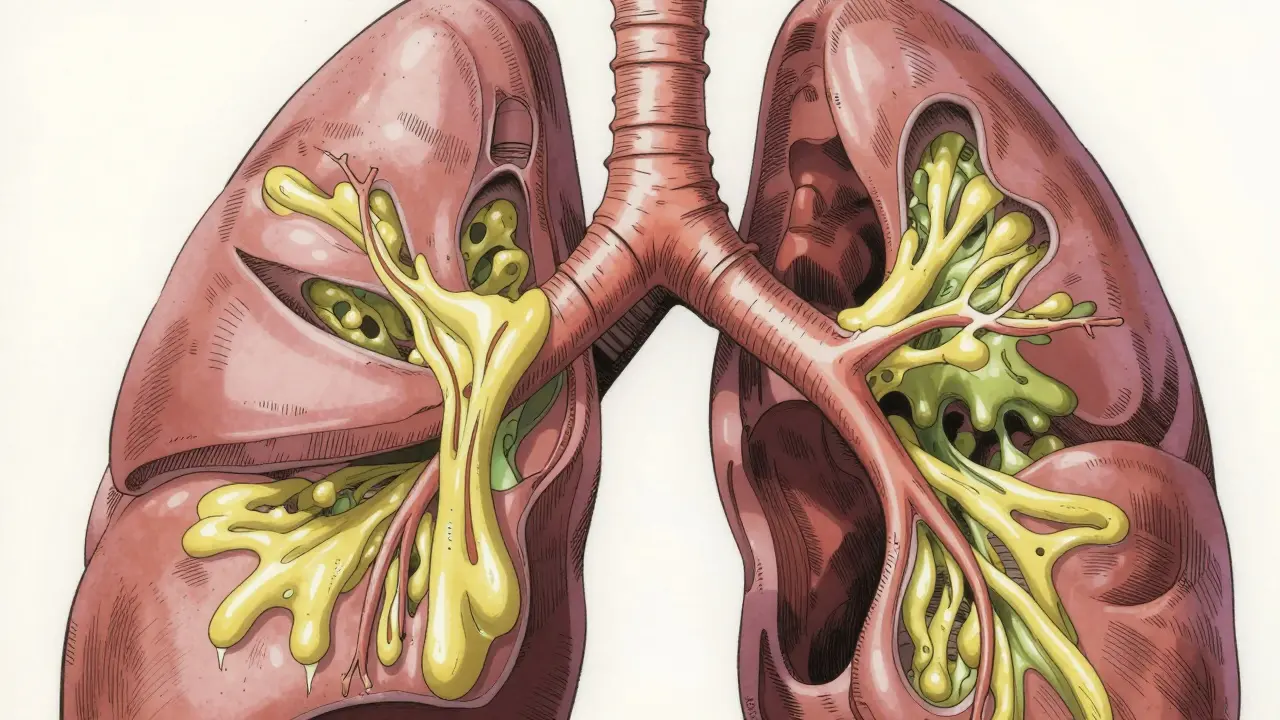
Imagine waking up every day feeling like your lungs are filled with heavy, sticky glue that just won't budge. For people living with Bronchiectasis is a chronic respiratory condition where the bronchial tubes become permanently widened and damaged. This structural change turns the airways into sort of "pockets" where mucus collects, making it a breeding ground for bacteria. If you've been struggling with a cough that never seems to go away, you're not alone. While the damage to the lungs is irreversible, the goal isn't a cure-it's about breaking the cycle of infection and inflammation to get your quality of life back.
The Vicious Cycle of Mucus and Infection
To understand why this condition is so stubborn, you have to look at the "vicious cycle." In a healthy lung, tiny hairs called cilia sweep mucus and debris out. In a lung with bronchiectasis, those hairs are damaged. When mucus stays trapped, it attracts bacteria. This leads to an infection, which causes more inflammation, which further damages the airway walls. Rinse and repeat.
The most telling sign is a chronic productive cough. We're talking about a significant amount of sputum-often 30mL or more every single day. Because of the white blood cells (neutrophils) fighting the infection, this phlegm usually looks yellow or green and can have a foul smell. If left untreated, this cycle can lead to a steady decline in lung function. In fact, untreated cases can see a drop in forced expiratory volume (FEV1) of up to 50mL per year, which is nearly double the rate of normal aging.
Mastering Sputum Clearance
If there is one thing every respiratory therapist will tell you, it's that sputum clearance isn't a "nice to have"-it's a necessity. If you don't get the mucus out, no amount of medication will fully solve the problem. The trick is moving from a standard cough to a more strategic approach.
The huff coughing technique is a game-changer for many. Unlike a hard, hacking cough that can collapse your airways, a "huff" is a forced expiration against an open glottis. It's like you're trying to fog up a mirror. To do it right, you need to master three phases: medium, low, and high lung volume huffs. It takes practice-usually about 12 supervised sessions with a pro-but it's the most effective way to move mucus from the small airways up to the larger ones where it can be spat out.
For those who need more help, technology steps in. You might use a Positive Expiratory Pressure (PEP) device, like the Aerobika, which creates resistance to keep airways open longer. For more severe cases, a high-frequency chest wall oscillation vest can be used. These vests vibrate the chest to loosen mucus, often clearing 35% more sputum than traditional manual physiotherapy.
| Method | How it Works | Typical Cost | Main Benefit |
|---|---|---|---|
| Huff Coughing | Forced exhalation (fogging a mirror) | Free | Immediate relief, no equipment |
| PEP Devices | Resistance during exhale | $150 - $300 | Portable, opens airways |
| Oscillating Vests | High-frequency vibration | $5,000 - $7,000 | Maximum mucus volume removal |

Using Antibiotics Wisely
Antibiotics in bronchiectasis aren't just for when you're sick; they're often used to keep you from getting sick in the first place. The goal is to keep the bacterial load low so the lungs don't get overwhelmed.
There are two main ways these are used. First, there's prophylaxis. Many patients take Azithromycin, a macrolide antibiotic, three times a week. This isn't just about killing bacteria; it also helps reduce the inflammation in the lungs. Data shows this can cut the frequency of flare-ups by about 32%.
Then there are inhaled antibiotics, such as Tobramycin. These are specifically used if you have a Pseudomonas aeruginosa infection, a stubborn bacterium common in damaged lungs. Inhaling the medicine puts it directly where it's needed, reducing colonization by up to 56%.
A word of caution: don't rely on antibiotics alone. If you take pills but skip your airway clearance, you're essentially just "cleaning the floor while the ceiling is still leaking." Over-reliance on drugs without clearing the mucus can lead to antibiotic-resistant bacteria, which makes future infections much harder to treat.
Thinning the Mucus: Nebulizers and Hydration
If your mucus is too thick to cough up, you need to change its consistency. This is where nebulized therapies come in. A common protocol involves using a 7% hypertonic saline solution. This salt-water mist draws water into the airways, thinning the mucus so it slides out more easily. Some patients also use dornase alfa, an enzyme that breaks down the DNA in the mucus, making it less sticky.
Beyond the machines, hydration is your best friend. If you're dehydrated, your mucus becomes thick and tenacious. Aiming for at least 2 liters of water a day is a simple but critical part of the routine. When you combine hydration with saline nebulization and a bronchodilator, you often see a 28% improvement in symptom relief compared to using a bronchodilator on its own.

Daily Living and Common Hurdles
Let's be real: the treatment burden for bronchiectasis is heavy. Spending 20 to 45 minutes a day on clearance routines, plus nebulizers and medications, is a lot to ask of anyone with a job or a family. Many people find the first two months frustrating as they learn the techniques.
To make it stick, try to integrate it into your day. Some find it easiest to do their clearance right after a nebulizer treatment when the mucus is thinnest. Others use apps to track their adherence. The most important thing is consistency. Those who stick to their daily routine have significantly fewer hospitalizations-up to 47% fewer per year-than those who only treat their symptoms when they feel a flare-up coming on.
Can bronchiectasis be cured?
No, the structural widening of the bronchial tubes is irreversible. However, the condition can be managed effectively. With a combination of daily airway clearance, hydration, and targeted antibiotics, most people can slow the progression of the disease and significantly reduce the number of lung infections they experience.
How do I know if my airway clearance is working?
The most immediate sign is the amount and consistency of the sputum you cough up. If you are successfully clearing your lungs, you should see a noticeable amount of mucus being expelled. If you feel "congested" but nothing is coming up, you may need to adjust your technique or increase your use of saline nebulizers to thin the secretions.
Why do I need antibiotics if I'm not currently sick?
This is called prophylactic treatment. In bronchiectasis, bacteria often live permanently in the damaged areas of the lungs. Low-dose, long-term antibiotics (like Azithromycin) help prevent these bacteria from multiplying and causing a full-blown exacerbation, which helps protect your remaining lung function.
Is a chest vest better than a handheld PEP device?
Vests are generally more powerful and can clear a larger volume of sputum, making them great for severe cases. However, handheld PEP devices are much cheaper, more portable, and for many patients, provide comparable symptom control. The best device is the one you will actually use every single day.
What happens if I stop my daily clearance routine?
Stopping your routine allows mucus to accumulate, which quickly leads to infection. Research shows that patients who only treat flare-ups have a much higher risk of permanent lung function decline compared to those who maintain a daily management plan. Consistency is the key to avoiding hospital visits.
Next Steps for Better Lung Health
If you've just been diagnosed, your first priority should be scheduling a few sessions with a respiratory therapist. Learning the a-b-c's of the huff cough from a pro is much more effective than trying to figure it out from a pamphlet. Start a simple daily log to track how much sputum you're clearing and whether your cough is improving.
For those already in a routine, consider a "tune-up." Many patients need re-education every six months because technique can slip over time. Ask your doctor if you're a candidate for newer treatments, such as inhaled gallium maltolate for stubborn infections, or if you should be integrating more hypertonic saline into your nebulizer routine to make your clearance sessions more productive.





Rauf Ronald
April 8, 2026 AT 14:50The huff coughing technique is honestly the gold standard for anyone starting out. I've seen so many people struggle with the standard cough and just exhaust themselves without moving any mucus. If you can't get to a therapist right away, try practicing in front of a mirror to really see that "fogging" effect. It makes a world of difference in how much you clear during your morning routine!
Darius Prorok
April 9, 2026 AT 02:33Pretty basic stuff here. Everyone knows that if you don't drink water your phlegm turns into cement. It's just common sense.
Benjamin cusden
April 11, 2026 AT 02:27While the mention of PEP devices is adequate, the post fails to elaborate on the specific pressure gradients required for optimal distal airway clearance. It is painfully obvious to anyone with a medical background that the efficacy of the Aerobika depends entirely on the patient's ability to maintain a consistent expiratory flow. The simplification of these mechanisms for a general audience is, as always, a necessary but disappointing compromise in technical accuracy.
Alexander Idle
April 12, 2026 AT 13:33Omg the sheer tragedy of spending 45 minutes a day just to cough! It's practically a full-time job. I can't even imagine the drama of trying to explain to a boss why you need a "mucus break" every few hours. Truly a nightmare scenario!
Del Bourne
April 12, 2026 AT 15:21Adding to the hydration point, some people find that adding a humidifier to their bedroom at night helps keep the secretions from thickening during sleep. It can make that first morning clearance session much more productive. Also, remember that the timing of your bronchodilator is key; using it right before your huffing exercises helps open the pipes and lets the mucus flow out more freely.
Toby Sirois
April 13, 2026 AT 03:01Most of you are just following orders without thinking. If you're just popping Azithromycin and not fixing your lifestyle, you're just delaying the inevitable. I've seen people ignore the root cause for years and then wonder why their lungs are shot. Wake up and actually commit to the work or stop complaining about the symptoms.
Stephen Luce
April 14, 2026 AT 04:10It really is a heavy burden to carry every day, especially when you're feeling exhausted. Just know that it's okay to have days where the routine feels overwhelming. You're doing the best you can with a tough condition.
Kathleen Painter
April 15, 2026 AT 08:50I think it's so important that we acknowledge how different everyone's journey is with this, because while the vest might be the gold standard for some, others might find a simple saline nebulizer and a bit of gentle movement to be enough to keep them stable. We should really be encouraging people to listen to their own bodies and find the rhythm that works for their specific lifestyle, whether that's doing the clearance in the shower to use the steam or finding a quiet corner at work where they feel safe and comfortable. It's all about creating a sustainable habit that doesn't feel like a chore, but rather a form of self-care that allows them to breathe easier and enjoy their day without the constant fear of a flare-up.
Windy Phillips
April 16, 2026 AT 01:52The lack of emphasis on the psychological toll is just... typical!!! It's not just about the sputum; it's about the crushing weight of a lifelong illness... and yet we just talk about "huffing"... how quaint!!!
jack hunter
April 16, 2026 AT 08:00antibiotics r just a bandaid for a deeper hole in the soul of the body... why do we trust chemicals more than the natural flow of the universe?? the more we try to control the mucus the more it controls us... its a paradoxical dance of sickness and science... totaly fake way to live
GOPESH KUMAR
April 17, 2026 AT 04:54The focus on technology is a distraction from the fundamental truth that the body is a mirror of the mind. These vests and devices are merely crutches for those who refuse to master their own breath. It is a classic case of modern medicine replacing discipline with machinery, which in the long run, only weakens the human spirit's resolve to heal itself through sheer will and awareness.
Jitesh Mohun
April 18, 2026 AT 13:51stop overthinking it just do the huffing and drink your water man its not that deep just follow the plan and stop whining about the time it takes
Nikhil Bhatia
April 19, 2026 AT 23:14Too much text. Just use a vest.