PPI & Clopidogrel Interaction Checker
Select the PPI medication you are currently taking to see its interaction profile with clopidogrel.
Note: This tool is for educational purposes based on the provided article. Always consult your physician before changing your medication regimen.
Imagine taking a medication to prevent a heart attack, only to find out that another common pill for heartburn is quietly stopping the first one from working. That is exactly what happens with the interaction between clopidogrel is an antiplatelet medication used to reduce the risk of heart disease and stroke by preventing blood clots and certain Proton Pump Inhibitors (PPIs). While PPIs are great for protecting the stomach, some of them act like a roadblock in the liver, preventing clopidogrel from turning into its active form. If the drug isn't active, your blood doesn't thin properly, and the risk of a cardiovascular event goes up.
Why the Interaction Happens: The CYP2C19 Problem
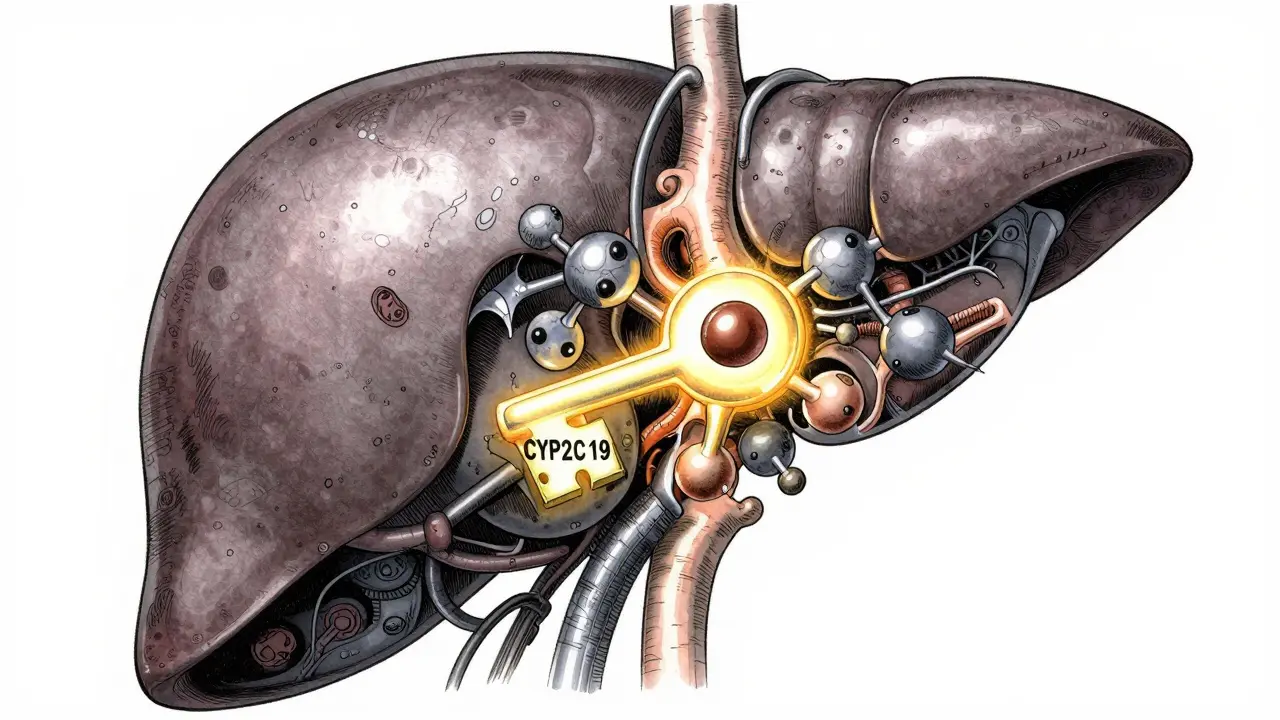
To understand this, we have to look at how clopidogrel works. It is a "pro-drug," meaning it is inactive when you swallow it. For it to actually stop platelets from sticking together, your liver needs to convert it using a specific enzyme called CYP2C19. Think of this enzyme as a key that unlocks the medication.
Here is the catch: many PPIs use that same "key" to be processed by the body. When you take both, the PPIs hog the enzyme, leaving clopidogrel stranded in its inactive state. This is called competitive inhibition. For example, high doses of omeprazole can slash the levels of clopidogrel's active metabolite by nearly 50%. This means the drug is in your system, but it isn't doing its job.
It gets even more complicated because of genetics. About 30% of people have a genetic variation called a loss-of-function polymorphism. These "poor metabolizers" already struggle to activate clopidogrel. When they add a PPI into the mix, the effect is compounded, significantly increasing the risk of major cardiovascular events.
Not All PPIs Are Created Equal
The good news is that not every heartburn medication causes the same level of interference. Some PPIs are "aggressive" inhibitors of the CYP2C19 enzyme, while others barely touch it. If you are on antiplatelet therapy, the specific brand of PPI you use matters immensely.
| PPI Medication | Inhibition Strength | Impact on Clopidogrel | Clinical Recommendation |
|---|---|---|---|
| Omeprazole | Strong | Significant reduction in activity | Avoid if possible |
| Esomeprazole | Strong | Significant reduction in activity | Avoid if possible |
| Lansoprazole | Moderate | Mild to moderate reduction | Use with caution |
| Pantoprazole | Minimal | Negligible effect on activation | Preferred choice |
| Rabeprazole | Intermediate | Moderate effect on peak levels | Acceptable alternative |
Data shows a stark contrast here. Omeprazole can reduce the antiplatelet effect of clopidogrel by nearly 39%, whereas pantoprazole shows almost no significant reduction. This is why the FDA has a black box warning specifically mentioning omeprazole and esomeprazole.
The Great Debate: Heart Health vs. Stomach Bleeding
Doctors are often caught in a tug-of-war when prescribing these drugs. On one hand, dual antiplatelet therapy (taking aspirin and clopidogrel together) increases the risk of gastrointestinal bleeding by about 50%. This makes a PPI almost necessary for many patients to prevent a stomach ulcer or a bleed.
On the other hand, if the PPI stops the clopidogrel from working, the patient might face a stent thrombosis-where a clot forms inside a heart stent. Some experts, like those involved in the TRITON-TIMI 38 trial, argue that this risk is too high to ignore. Others, such as the investigators of the COGENT trial, suggest that the actual increase in heart attacks is modest and that the benefit of preventing a massive GI bleed outweighs the risk.
The current consensus from the American College of Cardiology (ACC) suggests an individualized approach. Instead of banning PPIs entirely, the goal is to pick the "right" PPI. If a patient has a high risk of stomach bleeding (such as being over 65 or having a history of ulcers), a PPI is a must, but pantoprazole is the smarter bet.
Practical Strategies for Patients and Caregivers
If you or a loved one are taking these medications, there are concrete steps to minimize risk. First, review the specific PPI being used. If it is omeprazole or esomeprazole, talk to a doctor about switching to pantoprazole or dexlansoprazole.
If a switch isn't possible, some clinicians suggest staggering the doses. Taking the PPI in the morning and clopidogrel in the evening can help reduce the amount of time both drugs are competing for the same liver enzymes at their peak concentrations. While this isn't as effective as switching drugs, it's a better strategy than taking them at the exact same time.
For those at very high risk, genetic testing is an option. A CYP2C19 test (like the Roche Amplichip) can tell a doctor if you are a poor metabolizer. If you are, clopidogrel might not be the best drug for you regardless of whether you take a PPI. In those cases, a different antiplatelet like ticagrelor might be used, as it doesn't require the liver's "unlocking" process to work.
The Future of Antiplatelet Therapy
The medical world is moving toward drugs that bypass this liver bottleneck entirely. Ticagrelor is a prime example. Because it doesn't need to be activated by CYP2C19, it doesn't care if you're taking a PPI. Recent data shows it may even lower cardiovascular mortality more effectively than clopidogrel.
However, cost remains a massive barrier. Generic clopidogrel costs only a few dollars a month, while ticagrelor can cost hundreds. This economic reality means that for millions of people, managing the PPI interaction will remain the primary way to stay safe.
Can I take omeprazole with clopidogrel?
It is generally recommended to avoid this combination. Omeprazole strongly inhibits the enzyme CYP2C19, which is necessary to activate clopidogrel. This can make clopidogrel less effective, increasing your risk of blood clots. Talk to your doctor about using pantoprazole instead.
Which PPI is safest to use with clopidogrel?
Pantoprazole is widely considered the safest option because it has a minimal effect on the CYP2C19 enzyme. Dexlansoprazole is also often preferred over omeprazole or esomeprazole.
Does the timing of the doses matter?
Yes. If you must take a PPI that interacts with clopidogrel, staggering the doses (e.g., PPI in the morning and clopidogrel at night) may help reduce the competitive inhibition in the liver, though switching to a non-interacting PPI is the preferred solution.
What is a CYP2C19 polymorphism?
It is a genetic variation that affects how your liver processes certain drugs. People with a "loss-of-function" polymorphism produce an enzyme that doesn't work well, meaning they can't activate clopidogrel efficiently, making them more susceptible to the negative effects of PPI interactions.
Why do doctors prescribe PPIs if they interfere with heart meds?
Dual antiplatelet therapy significantly increases the risk of stomach ulcers and gastrointestinal bleeding. For many patients, especially the elderly or those with a history of ulcers, the risk of a severe bleed is considered more immediate and dangerous than the potential reduction in clopidogrel's effectiveness.





Sue Stoller
April 22, 2026 AT 01:35This is such a helpful breakdown! 🌟 It's so important to stay proactive about our health and just have those little chats with our doctors to make sure we're on the best path! Keep shining everyone! ✨💖
Rick Brewster
April 23, 2026 AT 16:05the sheer irony of the biological machinery being so fragile that a simple heartburn pill can derail a lifesaving treatment is truly a testament to the chaotic nature of human existence where we try to fix one leak only to accidentally open another floodgate in the liver we are essentially just chemistry sets with anxiety and bad posture if you really think about the systemic failure of the medical industrial complex to educate the masses on pharmacogenetics it becomes quite clear that we are just pawns in a game of trial and error played by people with fancy degrees
Chidi Prosper
April 25, 2026 AT 14:29Pantoprazole is definitely the way to go here. There's no reason to risk a stent thrombosis when a safer alternative exists right in the same drug class. Switch it now.
Dan Wizard
April 26, 2026 AT 21:42It is truly fascinating how the intricate dance of enzymes in the liver can dictate the efficacy of a life-saving medication, and while I find the concept of the CYP2C19 enzyme acting as a biological key to be an elegant metaphor, I cannot help but wonder if the widespread nature of these genetic polymorphisms means that a significant portion of the global population is essentially walking around with an inherent vulnerability to standard treatment protocols, which makes the availability of genetic testing like the Roche Amplichip not just a luxury but a fundamental necessity for personalized medicine in the modern age, provided of course that the healthcare system is equitable enough to provide such tools to everyone regardless of their socio-economic status.
Anastasios Kyriacou
April 28, 2026 AT 14:31too much readin... just take the pantoprazole and stop worryin about it lol
Divyanshu Giri
April 29, 2026 AT 05:44Big win for the smart pills! Just swap that med and feel the power! Super easy fix for a big problem!
Mayur Pankhi Saikia
April 29, 2026 AT 21:27The arugment that the COGENT trial proves the risk is "modest" is simply laughable...!! It ignores the catastrophice failure of a single stent thrombus in a high-risk patient...!! Truly a flaw in the logic of the authors!!
Sarah Watters
April 30, 2026 AT 03:18Probably just another way for Big Pharma to push the expensive ticagrelor. They make clopidogrel cheap so they can keep us dependent, then they tell us it doesn't work for 30% of us just to sell the hundred-dollar version.
Amy Fredericks
April 30, 2026 AT 16:06I think it's wonderful that we have options like pantoprazole to balance both heart and stomach health. It's all about finding that middle ground that works for each individual person.
Mel Glick
May 2, 2026 AT 14:25Actually, the cost barrier is a disgrace. We can't just "manage the interaction" when the safer drug is priced out of reach for the average person. It's a systemic failure, period.
Ally Warren
May 3, 2026 AT 11:31The paradox of the PPI is that it protects the vessel of the stomach while potentially endangering the vessel of the heart. We are always trading one risk for another in the pursuit of longevity.
Anantha Lakshmi
May 3, 2026 AT 13:56Exactly! Let's all encourage our families to check their prescriptions today! 🌈💪 Small changes make a huge difference in our health journey! ✨